| Back to Back Issues Page |
 |
|
Newsletter - New Secrets About Health and Wellness - Heart Attack, Stroke and Cholesterol November 17, 2013 |
Yours in Health and WellnessCholesterolIf you are new to this Newsletter and to the question of causes of heart and attack stroke you might want to quickly review the previous issue on Homocysteine where some of the key processes are summarized. Cholesterol was first isolated from gallstones in 1784. Since then 13 researchers have won the Nobel Prize for work centred primarily on cholesterol. But this issue of the Newsletter is about much more than cholesterol in all its various forms. There is lots of information so let’s begin with The Take-away. In the last Newsletter you learned about why you have to get your Homocysteine levels measured. In this one you’ll find out why you also need to get your LDL, VLDL and HDL-Cholesterols measured along with your Triglycerides and your Resistin. Cholesterol is not all bad news. Cholesterol is one of the fats in your blood. Your body uses it to make cell membranes, vitamin D and hormones. Specifically in the case of the very important secosteroid hormone, the so-called “Vitamin” D, sunlight acting on the 7-dehydrocholesterol in your skin converts it to cholecalciferol – Vitamin D3. Triglycerides while not a type of cholesterol, are types of fat found in the blood and are associated with excess weight, excess alcohol consumption and diabetes. Triglycerides should always be measured at the same time as cholesterols and homocysteine. In the 1950s and 1960s the race was on for a number of companies, each of which wanted to hit the mother lode, and create better health by finding some drug that would block at least one of the steps in the synthesis of cholesterol from acetyl-coenzyme A (CoA) in the body. The first commercially available drug, Triparanol, introduced in 1959 was withdrawn in the early 1960s because it caused cataracts. (1) Anytime a foreign substance is introduced into the body side effects are almost inevitable. This would be a challenge for all cholesterol -lowering drugs. By the 1980s and early 1990s the research on cholesterol was interpreted by the medical community as saying that ALL cholesterol is bad. That is ALL types of cholesterol were viewed as a causative factor for cardiovascular Disease (CVD). So the great goal of most doctors and of the medical establishment in the 1970s and 80’s was to lower ALL cholesterol. This was true even though John Gofman in 1949 at UC Berkeley, found not only that heart attacks correlated with elevated levels of blood cholesterol but also that the cholesterol correlated with heart attacks was contained in low density lipoprotein (LDL).(2) He also observed that heart attacks were less frequent when the blood contained elevated levels of high density lipoprotein (HDL).(3) Technically LDL and HDL are not cholesterol, but proteins that transport cholesterol to our cells. Cholesterol is neither water soluble nor blood soluble so it needs to be transported by a protein. So when we talk about cholesterol levels we are actually measuring the lipoproteins combined with cholesterol that transport cholesterol. Thus the research on cholesterol is really about which lipoproteins carrying cholesterol are good and which are bad; and what ratio should we have of the different lipoproteins for optimum cardio-vascular health.
TriglyceridesTriglycerides while not a type of cholesterol, are 3 types of fat found in the blood and are associated with excess weight, excess alcohol consumption, diabetes and CVD. Our lipoproteins also carry these three fats that make up what we call triglycerides: mono-unsaturated, saturated and poly-unsaturated. Triglycerides (TG) should always be measured at the same time as your lipoproteins (cholesterols) and homocysteine. They are an independent risk factor for CVD and their role in promoting CVD was first suggested by JR Moreton in 1947.(4)AFH Stalenhoef and J de Graaf noted in 2008 that studies showed “fasting triglycerides increase the adjusted hazard ratios for cardiovascular disease risk 1.7× (comparing upper with lower tertile), and nonfasting levels around 2.0×.” (5) A 2009 meta review by WB Kannel and RS Vasan noted that the “failure to catabolize triglyceride-rich lipoproteins (TRL) efficiently appears to be linked to accelerated atherogenesis since TRL appear to be proinflammatory, cause endothelial dysfunction , upregulate expression of endothelial adhesion molecules and promote macrophage chemotaxis. TRL are especially prone to enter the arterial wall where they are ingested by macrophages (analogous to oxidized LDL), to then become foam cells. Retention of these TRL in the vascular wall also traps the more atherogenic small LDL-Cholesterol particles”. (6)
Very Low Density Lipoprotein (VLDL) contains the highest levels of triglyceride. High levels of VLDL are linked to the risk of CVD, while large VLDL particles are associated with hypertension – high blood pressure. VLDL is typically estimated as a percentage of triglyceride. 5 to 30 mg/dL is considered a normal range.
Mayo Clinic (new window)
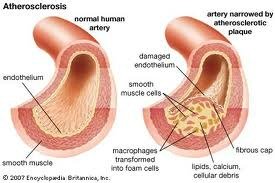
By 1997 it was found that the so-called bad “cholesterol”, LDL, is only bad once it is oxidized. An extensive review article concluded that antioxidants may very well reduce the risk of atherosclerosis by helping produce LDL that is resistant to oxidative modification. This in turn reduces the initial phases of “hardening of the arteries”, namely the fatty streak. Antioxidants also stabilize the arterial plaque where it is most likely to rupture (in the oxidized LDL laden foam cell layer of the plaque) and cause a heart attack. It may also reduce the size of the plaque thus reducing constriction or “narrowing” of the artery. (7) The same year it was reported that a high dose of antioxidants (800 IU of Vitamin E, 1000 mg of Vitamin C and 24mg of beta-carotene – provitamin A) reduced the susceptibility of LDL to oxidation in patients with cardiovascular disease. (8) This finding was reinforced by the results of a study reported in 2005. This study examined the relationship between oxidized LDL (oxLDL) and CVD/CHD. This study followed men initially assessed in 1989/90, 1994/95 and followed up in 1998. OxLDL was found in 88 men with incident CHD and in 258 age- and survey-matched controls. OxLDL concentrations were significantly higher in subjects who subsequently experienced an event compared with controls. Plasma oxLDL was the strongest predictor of CHD events compared with a conventional lipoprotein-cholesterol profile and other traditional risk factors for CHD. (9)
At the 2004 American Heart Association Annual Scientific Sessions presenters from Tufts – New England Medical Centre, reported on a meta-analysis of 17 major lipid lowering trials involving 44,170 patients and involving 3,869 fatal or non-fatal heart attacks. They found that the increase in HDL was the best predictor of decreased risk of heart attack, and clearly a better predictor than lowering LDL,.Their analysis also showed that there was no marked reduction in risk of heart attack until LDL was reduced by more than 30%.(10) Are there specific forms of LDL that are particularly bad? In other words do some forms of LDL contribute more to endothelial dysfunction and CVD than others? A 2002 study of 61 Japanese men with CVD (proven by angiogram) found that an increased number of Very Low Density Lipoprotein (VLDL) particles is strongly associated with CVD, independently of traditional risk factors or newly recognized lipoproteins that cause hardening of the arteries (atherosclerosis), such as Intermediate Density Lipoprotein (IDL) or small, dense LDL, in Japanese men.(11) The next Newsletter will investigate ways to control the levels of lipoproteins (“cholesterol”). But let’s look for a moment at one recent study. A summary article in 2010 on the history of cholesterol lowering drugs, particularly statins (including the most popular – Pfifers Lipitor) concluded that “no major adverse effects of lowering cholesterol were noted in any of the studies”. (12) That is a very interesting finding since it was known at least by 2004 (in a meta-analysis of 70 studies) that widely prescribed statin cholesterol lowering drugs (HMG CoA – reductase inhibitors) block the biosynthesis of cholesterol and CoQ10 and the decrease in both is related to the dose of the drug. Lowering cholesterol may be beneficial but lowering CoQ10 is not. Congestive Heart Failure (CHF) is linked to CoQ10 deficiency. CoQ10 levels fall dramatically after age 40. Thus the depletion of CoQ10 by statin cholesterol lowering drugs can worsen myocardial function in those with CHF and those over 40. This tragic scenario may well be prevented by using supplemental CoQ10 with all statins. (13) And this is something that should always be recommended by medical practitioners. Moreover CoQ10 is the source of energy in the mitochondria of every cell. So depletion of it is one side-effect we really want to avoid.
ResistinRecent research has identified resistin (“discovered” in 2001), a cysteine-rich signaling peptide, as a factor in obesity and in CVD. It is one of a class of cysteine-rich proteins. Research by Shirya Rashid, PhD at McMaster University, Faculty of Health Sciences recently “identified a novel role of resistin in directly increasing the levels of the pro-atherogenic lipid and lipoprotein components of the atherogenic dyslipidemia in humans –that is, elevated triglycerides and increased LDL particle concentration”. In brief she and her team have been able to demonstrate the functional link and process by which high levels of resistin are associated with CVD, particularly in the obese population. (14)Dr. Rashid notes that “a recent large population-based Framingham study found a highly significant positive association between circulating resistin levels and serum triglycerides”. Knowing that the major carrier of triglycerides in human serum is the circulating triglyceride-rich VLDL particles, she and her team were able to demonstratein vitro how resistin plays a role in liver VLDL production. The rate of liver LDL uptake and clearance is, moreover, regulated primarily by hepatocyte liver cell surface LDL receptors, Dr. Rashid demonstrated how resistin had a significant impact on this process. In lay terms, resistin, in vitro plays a role in determining the level of LDL. Rashid also noted that “resistin has been reported to induce endothelial dysfunction, one of the earliest impairments at the vascular wall in the atherosclerosis process”. She notes that Choy et al (15) found the causal relationship between resistin and atherosclerosis using In vivo research in rabbits. These findings about resistin are very interesting and suggest some positive potential for better control of the lipoproteins that effect endothelial dysfunction and lead to CVD. While some of the studies involved humans through in vitro (“test-tube”) studies, ultimately in vivo (in living humans) studies are needed. One study showed that resistin can be lowered significantly with supplementation of 2g of Vitamin C (ascorbic acid) over a 2 week period.(16) Exercise was also found to reduce resistin levels in Type 2 Diabetes patients. (17) This issue will be discussed more fully in the next Newsletter but these “treatments” are mentioned here to show that there seem to be readily accessible solutions.
The Take-AwayPractitioners should also examine other ways of:• Raising HDL-Cholesterol • Lowering elevated LDL-Cholesterol • Lowering elevated VLDL-Cholesterol • Lowering elevated Triglycerides • Lowering Resistin • Lowering Elevated Homocysteine • Maintaining Healthy levels of CoEnzyme Q10
The first efforts should always focus on lifestyle, nutrition and nutritional supplements. These are readily available in the medical literature and will be reviewed in the next Newsletter. Yours in Health and Wellness Roger
Footnotes1. Proc Jpn Acad Ser B Phys Biol Sci v.86(5); May 11, 2010 2. J. Biol. Chem 1949: 179, 973–979 3. Science 1950: 111, 166–171 4. Science August 1947 5. Curr Opin Lipidology 2008;19:355-361 6. Curr Opin Cardiol. 2009 July; 24(4): 345–350 7. N Engl J Med 1997; 408-416 8. J Amer Coll Cardiol 1997; 30(2):392-9 9. Circulation. 2005;112: 651-657 10. Circulation( 2004; 110: 227-239 11. Coron Artery Dis 2002 Aug;13(5):255-62 12. Proc Jpn Acad Ser B Phys Biol Sci v.86(5): 484-493 13. J Nutr Environ Med 2004; 14(1):17-28 14. Rheumatol Curr Res 2013, 3:1 15. J Am Coll Cardiol 2011: 57(1):99-109 16. PLoS Clin Trials. 2007 May; 2 (5): e17 17. Diabetes Care 2007(30)3: 719-721 |
| Back to Back Issues Page |